Diabetes remains one of the most widespread chronic diseases in the world. According to the International Diabetes Federation, more than 530 million people are currently living with diabetes, and this number continues to grow. Patients are concerned not only about blood sugar control but also about the possibility of truly influencing the course of the disease, reducing the risk of complications, and decreasing dependence on daily injections. That is why new therapeutic approaches, including stem cell treatment for diabetes, are attracting increasing attention as they undergo clinical trials and are evaluated for both effectiveness and safety in different patient groups.
Current Data on Type 1 Diabetes Treatment
Type 1 diabetes is associated with the destruction of pancreatic beta cells that produce insulin. The primary goal of research is to restore or replace these cells and reduce the need for daily injections.
According to recent international clinical studies:
- In some patients, after islet cell transplantation, insulin requirements decrease by 30–80%.
- In certain cases, temporary insulin independence is achieved for periods ranging from several months to 2–3 years.
- Glycated hemoglobin (HbA1c) levels decrease on average from 8–9% to 6–7%, significantly lowering the risk of complications.
However, there are also challenges:
- the need for immunosuppressive therapy;
- risk of cell rejection;
- high procedural costs.
Many patients report blood sugar fluctuations, nighttime hypoglycemia, and fear of complications. This explains why methods aimed at restoring natural insulin production generate strong interest.
Research in Type 2 Diabetes
Type 2 diabetes is far more common and is associated with insulin resistance and gradual pancreatic dysfunction. Clinical research in this group focuses on improving insulin sensitivity, reducing body weight, and preventing complications.
Key findings from recent years include:
- GLP-1 receptor agonists reduce HbA1c by 1–1.5% and decrease body weight by an average of 5–15%.
- SGLT2 inhibitors lower the risk of cardiovascular events by 20–30% in high-risk patients.
- Combination therapy reduces the likelihood of progression of chronic kidney disease.
This is important because many patients struggle not only with high glucose levels but also with obesity, hypertension, and atherosclerosis. A comprehensive approach supported by clinical evidence helps reduce the risk of heart attack, stroke, and kidney failure.
The Role of Cellular Technologies and Regenerative Medicine
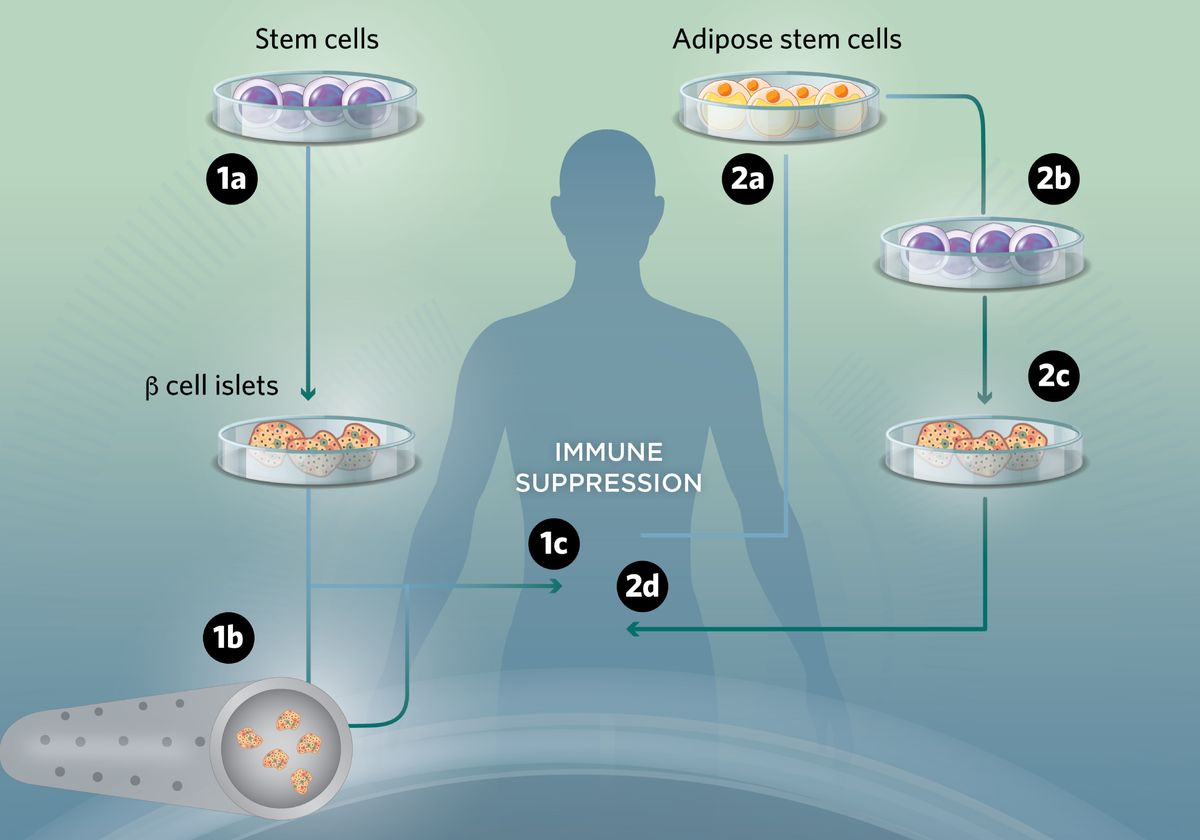
A separate and rapidly developing area is regenerative medicine. Research involving stem cells is focused on:
- Creating new beta cells from pluripotent cells;
- Protecting cells from autoimmune attack;
- Implanting encapsulated cells without the need for long-term immunosuppression.
In early-phase clinical trials, some patients have shown:
- stabilization of blood glucose levels;
- reduced frequency of hypoglycemia;
- decreased insulin dosage requirements.
However, these methods are still under active investigation. They require strict patient selection and long-term monitoring to confirm safety and durability of results.
Prevention of Complications: What Long-Term Studies Show
Large observational studies have demonstrated that glucose control is directly linked to the risk of complications. A 1% reduction in HbA1c lowers the risk of microvascular complications by approximately 30–35%.
The most common complications include:
- diabetic retinopathy;
- nephropathy;
- neuropathy;
- cardiovascular diseases.
Patients often underestimate the importance of regular monitoring until they experience vision problems or neuropathic pain. Clinical evidence clearly shows that early treatment adjustments and consistent monitoring of glucose, lipid levels, and blood pressure significantly extend active and healthy life expectancy.
Diabetes is not a sentence, but it is a chronic condition that requires a systematic approach. Clinical research demonstrates real progress: new medications are emerging, monitoring technologies are improving, and cellular therapies are advancing. At the same time, the foundation remains unchanged — regular monitoring, adherence to medical recommendations, and early intervention. The combination of evidence-based medicine and active patient involvement provides the best long-term outcomes and reduces the risk of severe complications.